Consultation Process
If you develop problems of your cervical spine, your neck, you may experience symptoms due to a damaged disc or bone spurs putting pressure on your spinal nerve or spinal cord.
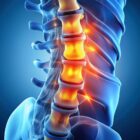
As we age, the disc space between the bones of our cervical spine will degenerate. Like other joints of our body, wear and tear of the disc space can lead to neck pain. The damaged disc becomes painful when we move our necks. This degeneration leads to a herniated disc or bone spurs to develop. These changes narrow the channels of the cervical spine and put pressure on spinal nerves, nerve roots, and spinal cord.
A variety of symptoms can develop from this irritation of the nerves, including:
- Neck pain that travels into the shoulder blade and arm
- Arm numbness, tingling, and/or weakness
- Poor hand coordination
- Walking difficulty
- A sense of urgency during urination
If you experience any of these issues, it is best to seek medical advice from a spine surgeon, particularly one who is familiar with conditions related to the cervical spine.
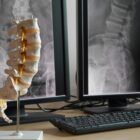
During your consultation, the spine surgeon should take a careful history and perform a detailed neurological exam. Your imaging, typically a cervical MRI and X-rays, should also be evaluated.
Always remember that physicians should treat patients, not X-rays or MRI’s.
Not every abnormality in an image may lead to symptoms or require treatment. Your spine surgeon should provide a clear explanation as to how abnormalities on your imaging are causing your symptoms. Do not be afraid to ask questions! This is your body; you need to understand your condition.
Appropriate treatments and the expected outcome of those treatments should be discussed.
Conservative care is often the first alternative. Utilizing medications to control pain, such as non-steroidal anti-inflammatory drugs (Advil for instance), and physical therapy are common treatments. Physical therapy is intended to improve your neck motion and posture and strengthen your muscles. If pain persists, an injection of the cervical spine may be appropriate.
If conservative care fails, or if you have significant neurological deficits, surgery is often indicated. One of the more common surgeries performed for a damaged or herniated disc of the cervical spine is an anterior cervical discectomy and fusion (ACDF).
If your spine surgeon recommends ACDF surgery, a detailed discussion of the procedure should be provided, including risks, benefits, and consequences.
If you decide to undergo ACDF surgery, you will need to be medically cleared by your primary care doctor. Your medical history and medications will be reviewed and potentially modified prior to surgery. For instance, if you take blood thinners, you may need to stop to safely undergo ACDF surgery.
It's time to get back
to doing what you love.
Procedure
Your spine surgeon should provide a clear description of a cervical discectomy and fusion.
The following is a list of steps involved with ACDF surgery:
- Incision to front of the neck
- Dissection to the spine
- Removal of damaged disc and bone spurs
- Placement of bone graft, metal plate and screws
- Incision closure
The procedure is performed in an operating room under general anesthesia.
The incision is usually hidden in a crease along the neck. The disc spaces that require surgery are identified. An anterior cervical discectomy is performed, removing the herniated disc and bone spurs. This will relieve the pressure and irritation on the spinal cord and nerve roots.
The space created by removing the damaged disc is filled with a bone graft.
The bones are then secured with a metal plate and screws, creating the spinal fusion. The bone graft heals to the vertebrae, providing long-term stability of the spine.
The incision is closed with absorbable sutures, under the skin. There are no sutures to remove. You are woken from anesthesia and taken to the recovery room for observation.
Post-Op
Following ACDF surgery, a short stay in the recovery room is required.
Patients are typically either discharged the same day as the procedure or spend one night in a hospital. It depends on how many damaged discs are removed.
Recovery/Follow-up
Your spine surgeon and their staff should provide clear discharge instructions. However, you should never hesitate to contact your surgeon if you have any questions.
A sore throat and some swallowing difficulties are common during the first week or two following ACDF surgery. A rigid collar may be required if recommended by your spine surgeon.
Medications to address post-operative discomfort will be prescribed. You may gradually increase your activities, but athletics or strenuous exercise should initially be avoided.
Typically, you will see your spine surgeon about a month after surgery.
Your condition will be reviewed, and X-rays evaluated. Depending on your neurological condition, physical therapy may be started immediately after discharge or later during your recovery. Periodic follow-up with X-rays will be performed for the first year.
Most patients will resume all their normal activities within 3 months.

About Dr. Michael G. Kaiser
Dr. Michael G. Kaiser is a nationally recognized neurosurgeon in North Jersey and is a proud member of Neurosurgeons of New Jersey, practicing out of their Ridgewood office conveniently located on East Ridgewood Avenue. Dr. Kaiser specializes in complex and minimally invasive spine surgeries.