Stereotactic Radiosurgery for Brain Metastases in NSCLC
Brain metastases present a complex challenge in the treatment of non-small cell lung cancer (NSCLC). As lung cancer frequently spreads to the brain, managing these metastases effectively is crucial.
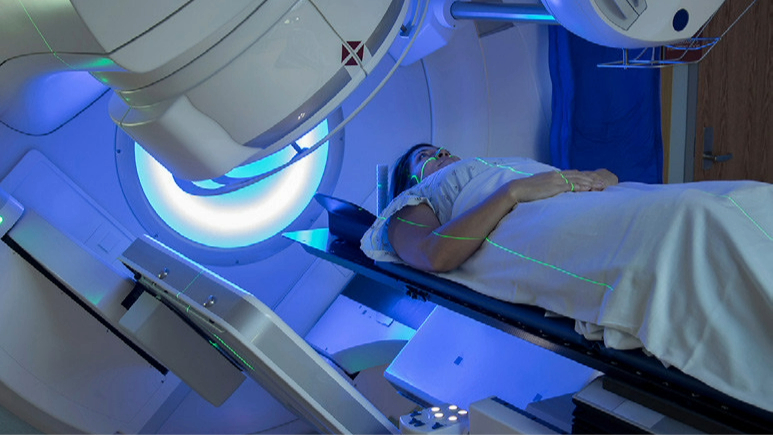
Stereotactic Radiosurgery (SRS) has become a pivotal treatment option, providing targeted and precise brain radiation therapy. This article aims to highlight the role of stereotactic radiosurgery in the treatment of brain metastases for NSCLC patients. It will provide insight into the benefits, risks and impact on patient care.
Understanding NSCLC and Brain Metastases
Non-small cell lung cancer is the the most common type of lung cancer. It often metastasizes to other body parts, including the brain.
What are Brain Metastases?
Brain metastases occur when cancer cells from the lung travel to the brain, posing significant health challenges and impacting a patient’s prognosis and quality of life.
The Critical Role of Magnetic Resonance Imaging (MRI)
In diagnosing and treating brain metastases, Magnetic Resonance Imaging (MRI) is indispensable. MRI scans provide detailed images of the brain, enabling physicians to accurately locate and assess metastatic brain tumors. This precise imaging is crucial for planning SRS, ensuring targeted treatment and maximizing effectiveness.
Gamma Knife Technology in SRS
The Gamma Knife is a specialized form of SRS designed specifically for brain conditions. This technology delivers a high dose of radiation directly to brain tumors with pinpoint accuracy, minimizing exposure to surrounding healthy brain tissue in order to spare the normal brain.
It is particularly beneficial for patients with brain metastases, offering a less invasive yet effective treatment option.
SRS Versus Traditional Brain Radiation Therapy
Stereotactic radiotherapy differs significantly from traditional brain radiation therapy. Traditional whole brain radiation therapy involves multiple sessions over several weeks, while SRS usually delivers a single, potent dose of radiation directly to the tumor.
This approach shortens the overall treatment duration and reduces the risk of damage to normal, healthy brain tissue. In addition, the use of stereotactic radiosurgery has been shown to reduce the risk of cognitive and learning deficits associated with whole brain radiation treatments, thereby improving quality of life
It's time to get back
to doing what you love.
Tackling Multiple Brain Metastases with SRS
Treating patients with multiple brain metastases presents unique challenges. SRS’s precision allows targeted treatment of each metastatic site, effectively reducing tumor burden and improving local control rates. This is especially pertinent in NSCLC, where the spread of multiple metastases to the brain is common.
Effectiveness of SRS: Local Control Rates and Overall Survival
SRS has shown impressive efficacy in managing the growth and spread of metastatic tumors within the brain. Studies indicate that SRS can positively influence overall survival rates in patients with NSCLC who develop brain metastases.
Managing Side Effects and Prioritizing Quality of Life
SRS is generally well-tolerated, with some patients experiencing manageable side effects such as temporary swelling, fatigue, or mild headaches. The benefits of SRS in preserving the patient’s quality of life are significant, allowing most individuals to maintain their usual activities with minimal interruption.
The Evolving Landscape of Radiation Oncology in NSCLC
Radiation oncology is pivotal in treating brain metastases from NSCLC. The field is continually evolving, with oncologists working alongside neurosurgeons, medical oncologists, and other specialists to develop personalized and effective treatment plans. This multidisciplinary approach is essential for optimizing patient outcomes in the face of complex metastatic diseases.
Staying Informed with Current Research
Keeping abreast of the latest research is crucial for healthcare professionals and patients alike. Recent studies and publications, notably in the Journal of Neurosurger and PubMed offer valuable insights into the effectiveness and safety of SRS in treating brain metastases from NSCLC.
Advances in SRS Technology and Patient Care
Technological advancements in SRS continue to refine its precision and effectiveness. Improvements in imaging techniques, radiation delivery systems, and patient care protocols promise even more accurate treatments, reduced side effects, and improved outcomes. These developments are particularly relevant for NSCLC patients, where the need for precise and minimally invasive treatments is paramount.
Patient Selection and Personalized Treatment Planning
Not all NSCLC patients with brain metastases are suitable candidates for SRS. Factors influencing eligibility include the size, number, and location of brain metastases, as well as the patient’s overall health and treatment history. Personalized treatment planning, considering these factors, is crucial for achieving the best possible outcomes.
The Future of SRS in Managing Brain Metastases
The future of SRS in treating brain metastases looks promising. Continued research and technological innovation are expected to enhance its efficacy and accessibility. This progress holds the potential for even more targeted treatments, fewer side effects, and better quality of life for patients with NSCLC and brain metastases.
Conclusion
Stereotactic Radiosurgery stands at the forefront of modern cancer care, offering a highly effective, targeted approach for treating brain metastases in non-small cell lung cancer patients. Its precision, minimal invasiveness, and ability to spare the mornal brain to preserve quality of life make it a vital component of comprehensive cancer treatment.
For patients and caregivers, understanding the nuances of SRS is essential for informed decision-making. It’s important to consult with healthcare professionals for personalized advice and treatment planning.
This article is for educational purposes only and is not a substitute for professional medical advice. Always consult your healthcare provider for personalized medical care.

About Dr. William S. Cobb
Dr. William Cobb is an accomplished neurosurgeon in North Jersey and a proud member of Neurosurgeons of New Jersey, practicing out of their Ridgewood office conveniently located on East Ridgewood Avenue. During his Neurological Surgery residency, he became passionate about the development and treatment of brain tumors affecting the brain and spine. Dr. Cobb uses state-of-the-art technology for surgical intervention in the treatment of tumors of the brain and spine including Gamma Knife radiosurgery. He has vast experience in using modern minimally invasive surgery for the treatment of degenerative spine and intervertebral disc disease. Dr. Cobb serves as the Director of Neurosurgical Oncology at Valley Hospital. He's accepting new patients.
Recent Posts: