Herniated Disc Treatment Options Explained
Understanding the cause and symptoms of a herniated lumbar disc can help to determine the best treatment option for your condition.
What is a herniated disc?
A herniated lumbar disc is a common cause for low back and sciatic-type leg pain also known as sciatica. Thankfully, most herniated disc management requires only conservative treatment. In some cases, surgery may be necessary
What causes a herniated disc?
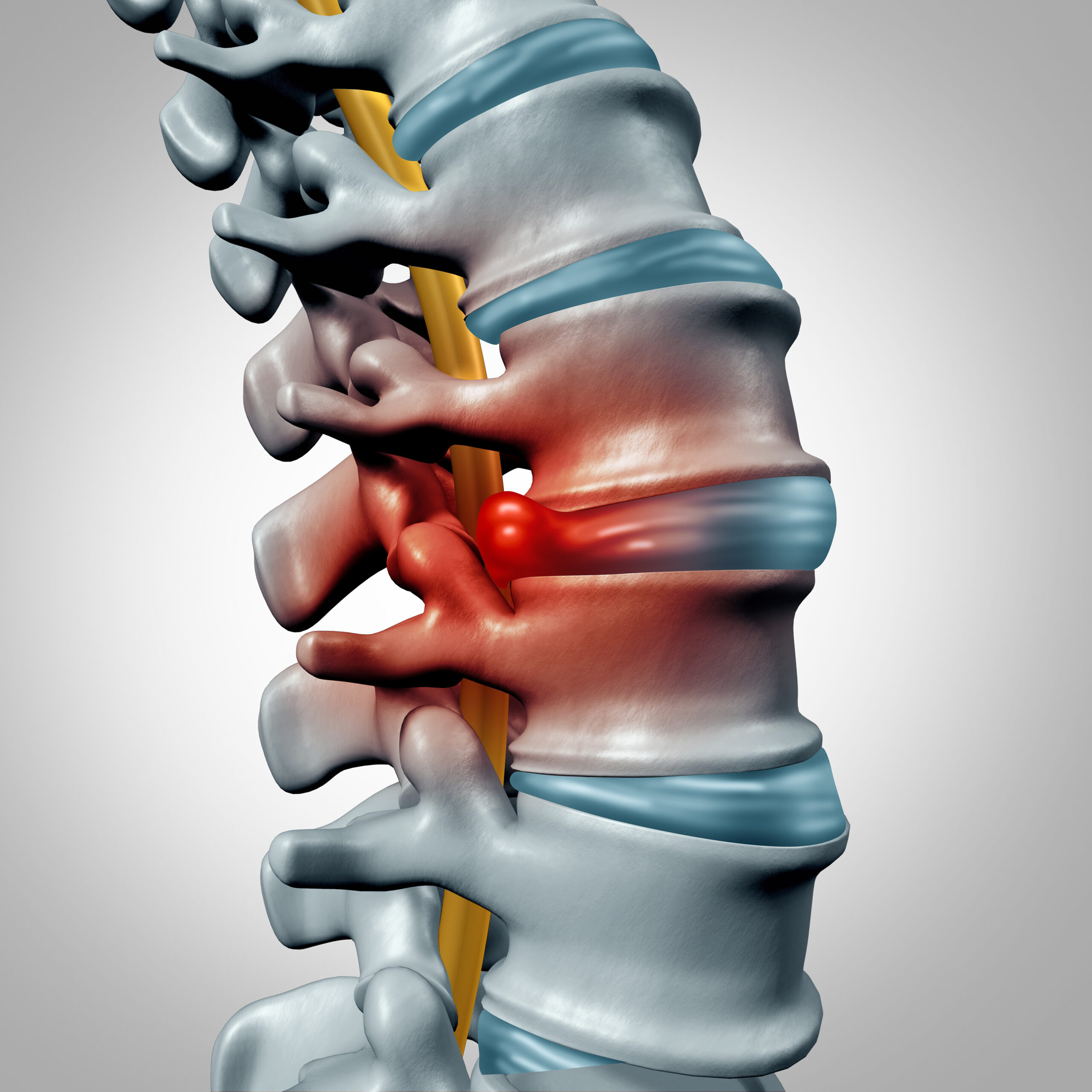
In between each of the bones in the lumbar spine, an intervertebral lumbar disc acts as a shock absorber to cushion the spinal column. Through an acute trauma or chronic degenerative spine changes, a piece of the disc can break off and “herniate” out to put pressure on or pinch the nerve.
Symptoms of a Herniated Disc
The symptoms of a herniated disk can cause pain and or even neurological symptoms. Typical symptoms are back pain and sciatic-type nerve pain with burning or electric-like pain running down the leg.
Symptoms will often originate in the lower-back or buttocks and can run down the back or side of the leg. In some cases, the pain may go all the way down to the foot. The pain can be experienced as numbness in the leg or may feel like an electric shock that is severe whether you stand, walk, or sit.
Less commonly, significant neurological symptoms may exist such as leg or foot weakness. Some patients have trouble lifting the foot when walking or standing on the ball of the foot, this condition is known as foot drop. In rare circumstances patients may experience the loss of bladder or bowel control.
Herniated Disc Treatment
In most cases of lumbar disk herniation, the disc will heal, and the pain will get better on its own. Pain can be quite significant initially but in greater than half of cases the pain will subside after a few weeks. If the pain does not ease after a few weeks, conservative treatment should be considered.
Conservative Management:
Most patients with lumbar herniated disc can be managed with conservative treatment options. Conservative management involves non-surgical treatments such as physical therapy, anti-inflammatory drugs, muscle relaxers or nerve medications may be prescribed.
Physical Therapy: Physical therapy is often the first line of treatment for patients with lumbar herniated disc. It focuses on strengthening the supporting muscles, improving flexibility, and promoting proper posture. Physical therapists utilize different techniques, including manual therapy, stretching exercises, and core stabilizing exercises, to reduce pain and improve functionality.
Medications:
Nonsteroidal anti-inflammatory drugs (NSAIDs) and muscle relaxers are commonly prescribed for pain relief and inflammation associated with lumbar herniated disc. Medication to treat nerve pain may also be prescribed.
Epidural Steroid Injections (ESIs)
Pain that is persistent, intolerable, and unresponsive to treatment, or accompanied by neurological symptoms, may require (magnetic resonance imaging) an MRI.
The MRI results will determine if a patient would benefit from an epidural steroid injection. This injection is used to reduce inflammation and symptoms in the area of the herniated disc. In some instances, a second or even third epidural steroid injection may be attempted to treat pain.
ESIs involve injecting corticosteroid medication into the epidural space surrounding the affected nerve root. This procedure aims to reduce inflammation and provide temporary relief from pain. ESIs can be particularly effective when combined with physical therapy to optimize outcomes.
In some cases, pain medications may be necessary to treat severe pain during the initial few days. After that, symptoms should start to subside. Bed rest or physical therapy may also be prescribed to help with healing.
Surgical Treatment
If symptoms last for long periods of time or neurological symptoms worsen, patients may benefit from surgical treatment such as lumbar microdiscectomy.
Lumbar Microdiscectomy is a minimally invasive surgical procedure. Its purpose is to remove the herniated portion of the disc. This alleviates pressure on the spinal cord or nerves.
It is considered the gold standard treatment for patients with severe or persistent symptoms that have not responded to conservative measures. Surgery typically takes 60-90 minutes and is performed on an outpatient basis. Microdiscectomy offers high success rates, minimal tissue disruption, and a relatively short recovery time.
How it is done
A small incision is made in the back above the level of the disc herniation. A small tubular retractor is placed over the disc and the operative microscope is brought into the field to assist with visualization. A small bony window is opened to expose the affected nerve root.
The disc herniation is exposed and then removed to completely decompress the pinched nerve. Once the incision is closed, the patient is observed for a short period of time and then goes home that day. The results of lumbar microdiscectomy are usually excellent and patients get rapid relief of symptoms.
What to expect after surgery
Most patients can go home just a few hours after surgery.
After the surgery, you may notice some limitations in mobility. It is crucial to follow your doctor’s instructions regarding movement and positioning. You may need assistance with activities such as sitting up, standing, and walking initially. Gradually, as you regain strength and mobility, you will be able to perform these activities more independently.
During the recovery period at home, your pain level will gradually decrease. Your doctor may prescribe pain medications to be taken as needed. As you begin to feel better, you can gradually reduce the use of pain medications, and transition to over-the-counter options as recommended by your doctor.
Engaging in light activities and gentle movements is an essential part of the recovery process. Walking is generally encouraged as a low-impact exercise that promotes blood circulation and helps prevent blood clots. However, it is important to avoid strenuous activities, heavy lifting, and bending or twisting motions for the initial weeks following surgery.
It's time to get back
to doing what you love.
Return to Normal Activities
The timeline for returning to normal activities, including work, varies from patient to patient. It is important to gradually reintroduce activities based on the guidance of your doctor. In general, individuals with sedentary desk jobs may be able to return to work within 4-6 weeks after surgery.
If your job involves heavy lifting, repetitive motion, or prolonged standing, it may take longer to regain strength and mobility. Your surgeon and healthcare team will assess your progress and provide specific recommendations regarding the appropriate time to return to work, to make sure that your recovery is not compromised.
It’s essential to communicate with your employer about any necessary accommodations or modifications that may be required during the transition back to work. Remember to prioritize your healing and gradually increase your activity level to prevent any setbacks in your recovery process.
A lumbar microdiscectomy is a surgery that aims to reduce pain and symptoms. However, even when the surgery is successful, some people may still have residual symptoms. This can include occasional episodes of mild pain or numbness. It is crucial to communicate any persistent or worsening symptoms to your surgeon for appropriate evaluation and management.
There is no need to suffer in pain-contact our office today to schedule a consultation with one of our doctors.

About Dr. William S. Cobb
Dr. William Cobb is an accomplished neurosurgeon in North Jersey and a proud member of Neurosurgeons of New Jersey, practicing out of their Ridgewood office conveniently located on East Ridgewood Avenue. During his Neurological Surgery residency, he became passionate about the development and treatment of brain tumors affecting the brain and spine. Dr. Cobb uses state-of-the-art technology for surgical intervention in the treatment of tumors of the brain and spine including Gamma Knife radiosurgery. He has vast experience in using modern minimally invasive surgery for the treatment of degenerative spine and intervertebral disc disease. Dr. Cobb serves as the Director of Neurosurgical Oncology at Valley Hospital. He's accepting new patients.