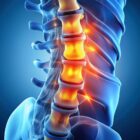
Cauda equina syndrome is a potentially serious neurological disorder caused by pressure on the cauda equina, a collection of nerves at the base of the spine that govern sensation and function in the lower limbs, bladder and bowels. Cauda equina syndrome can have a rapid onset with sudden severe symptoms, but it can also develop slowly, with early symptoms that often mimic other conditions. Recognizing these early symptoms is essential for a prompt diagnosis and appropriate treatment by experienced neurosurgeons in northern New Jersey.
What is Cauda Equina Syndrome?
The cauda equina (Latin for “horsetail”) is a cluster of nerves and nerve roots in the lower or lumbar, area of the spine that does indeed resemble the tail of a horse. These nerves control bowel and bladder functions as well as movement and sensation in the legs and feet. When those nerves are compressed, they lose the ability to control those functions, which causes weakness, numbness or paralysis in the lower extremities and bowel, bladder and sexual dysfunctions.
Pressure on the cauda equina can come from a variety of causes. The most common of these is a severely herniated disc that bulges outward and compresses nerves. Cauda equina syndrome can also be caused by other spinal conditions such as spinal stenosis or the bone disease osteoporosis. Tumors, infections and inflammation, and trauma to the lower back can also create pressure on the cauda equina. When symptoms appear, prompt treatment is essential, since cauda equina syndrome can leave patients with long-term bowel and bladder problems, leg weakness or paralysis.
Recognizing Early Symptoms of Cauda Equina Syndrome
Cauda equina syndrome manifests in two ways: a rapid development of severe symptoms or a slow and gradual onset with symptoms that gradually worsen over time. Symptoms of rapid onset cauda equina syndrome include leg and foot numbness and weakness, back pain, and bowel and bladder problems such as incontinence or retention. When that happens, immediate medical attention is essential to remove the source of pressure and give nerves the best chance to heal.
However, when the cause of pressure on the cauda equina develops gradually, such as from a slowly and steadily eroding lumbar disc or developing tumor, these early symptoms can be intermittent and vary in severity, so that they can be mistaken for other kinds of back problems or conditions that affect bowel and bladder functions. Early symptoms of cauda equina syndrome can include:
- Lower limb weakness and intermittent changes in sensation, such as numbness
- “Saddle anesthesia” – loss or diminished sensation in areas where a person would sit on a saddle
- Urinary and/or bowel problems, such as retention or incontinence
- Unexplained sexual dysfunctions, such as erection problems or loss of sensation
- Referred pain
- Poor tendon reflexes
Because these symptoms can also indicate many other conditions, cauda equina syndrome can be misdiagnosed and treated with inappropriate protocols such as medications for urinary issues and back pain, or manipulations such as chiropractic and physical therapy. These approaches can create more pressure on the cauda equina and worsen symptoms.
It's time to get back
to doing what you love.
Causes of Cauda Equina Syndrome
Cauda equina syndrome can be caused by a number of health conditions and events that lead to pressure on the nerves of the cauda equina.
Lumbar Disc Herniation
The most common of these is a massive disc herniation in the spine’s lumbar region. The spinal column contains a series of soft, flexible discs that act as cushions and “shock absorbers” between the bones, and these discs can herniate, or push outward from their original position due to circumstances such as aging and spinal injuries and conditions. When a disc in the lumbar region herniates, it bulges outward and can put pressure on the nerve roots of the cauda equina.
Lumbar Spinal Stenosis
Less often, cauda equina syndrome can also be caused by spinal conditions such as lumbar spinal stenosis, in which the spinal canal becomes narrow and causes pressure on nerves or trauma to the lumbar area.
Spinal Cancer
Cancer can also cause cauda equina syndrome when a tumor in the lumbar area begins to put pressure on the cauda equina.
Infection/Trauma
Infection o inflammation of the spine can also cause swelling and pressure on the nerves, and so can trauma from injury to the lower back in an accident, violent incident, or fall.
Osteoporosis
Rarely, osteoporosis, a degenerative bone disease, can cause fractures in the vertebrae that put pressure on the cauda equina.
Congenital Conditions
Some congenital conditions such as arteriovenous malformations can also create conditions that compress the nerves of the cauda equina.
Regardless of the cause, cauda equina syndrome needs immediate treatment to address the reason for compression of the cauda equina, and restore functioning to the lower body, bowels and bladder.
Diagnosing Cauda Equina Syndrome
Diagnosing cauda equina syndrome starts with a neurological examination and a detailed medical history, in order to determine when symptoms started and how they manifest over time. Although many of the early symptoms of cauda equina syndrome are similar to other conditions, the combination of leg weakness and numbness and bladder dysfunction can help to distinguish this syndrome from other spinal problems or a separate bladder disease.
If a patient has symptoms that suggest cauda equina syndrome, imaging tests such as MRI and CT scans are used to identify the source of pressure on the cauda equina. Neurologists may also order a myelogram, in which dye is injected into the spine and tracked with imaging technology to identify blockages.
Cauda Equina Syndrome Treatment Options
Treatment for cauda equina syndrome focuses on relieving the pressure on the nerves of the cauda equina – a procedure called spinal decompression surgery. During this procedure, an incision is made in the back at the site of the compression, so that neurosurgeons can locate and remove herniated discs, bone fragments, or tumors that could be pressing on the cauda equina. If the pressure is caused by infection or inflammation, medications can also be used to treat those issues. If the pressure is caused by a tumor, radiation and chemotherapy may also be needed after surgery.
Recovery from spinal decompression surgery typically requires a hospital stay of up to five days, and recovery at home can take four to six weeks, as patients gradually resume normal activities. But damaged nerves can take considerable time to heal, so leg weakness and bowel and bladder problems can continue for months or longer. In some cases, too, these problems can become permanent.
Prompt treatment to decompress the cauda equina provides the best chance for recovery of sensation and functioning in the affected areas. But if early symptoms are mistaken for other kinds of health problems, treatment can be delayed, and inappropriate treatment options that involve manipulations of the spine can even increase the pressure on the cauda equina.
The early symptoms of cauda equina syndrome can be intermittent, vary in intensity, and resemble symptoms of other conditions. An accurate diagnosis is essential for prompt treatment. In the tristate area, your New Jersey neurosurgeons can identify the early symptoms of cauda equina syndrome and create the best treatment plan for you and your unique circumstances.

About Dr. Gaetan Moise
Dr. Gaetan Moise is an accomplished neurosurgeon in North Jersey and is a proud member of Neurosurgeons of New Jersey, practicing out of their Ridgewood office conveniently located on East Ridgewood Avenue. His compassionate evidence-based, results-driven approach is guided by his desire to help patients achieve happy, pain-free lives through non-surgical and appropriate surgical solutions. Dr. Moise’s techniques are influenced by the advancements in minimally invasive surgery technology as well as advances in the understanding of the intricacies of the nervous system, brain, and spinal cord. Dr. Moise is a member of The Congress of Neurological Surgeons and the American Association of Neurological Surgeons. He is accepting new patients.