Pituitary Tumor Surgery – From Diagnosis to Recovery
What is the Pituitary Gland?
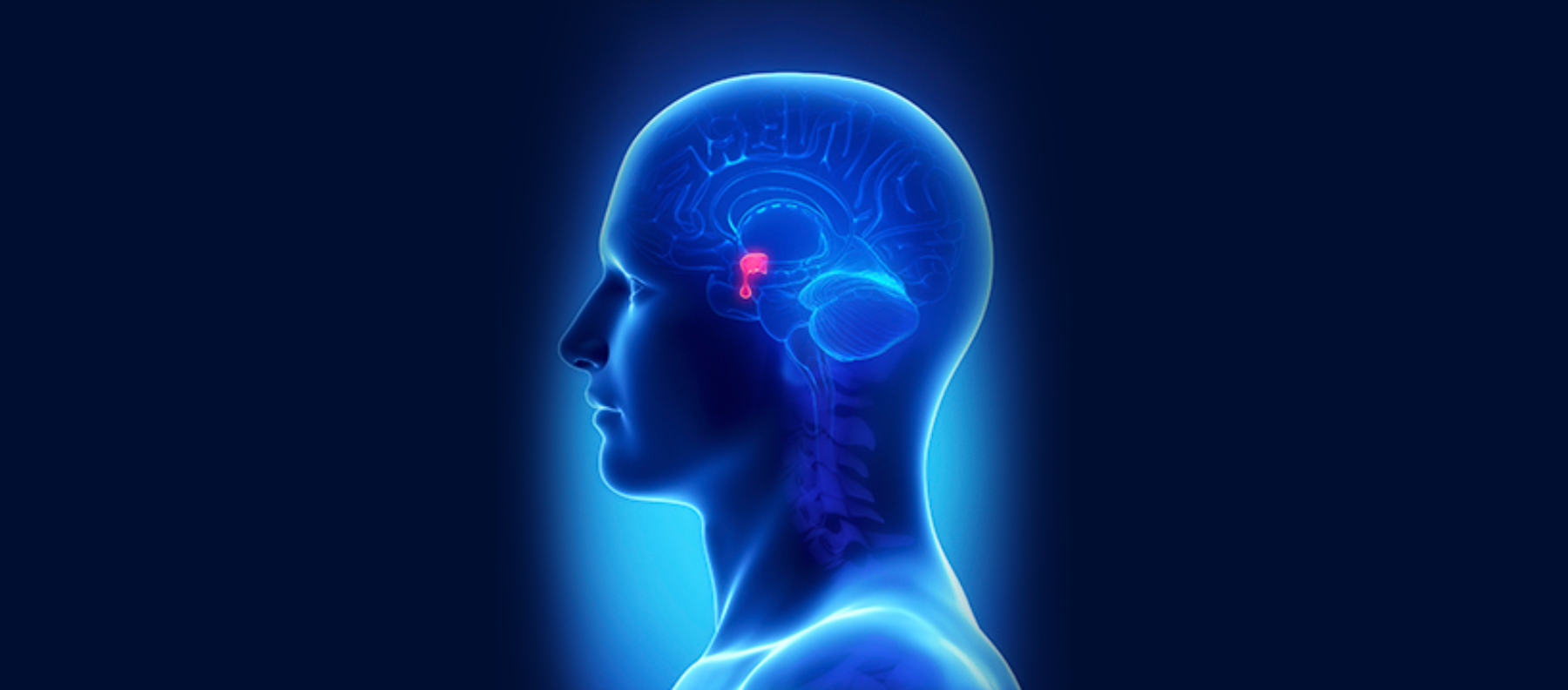
The pituitary gland, nestled at the base of the skull, acts as the master regulator for hormone production in the body. It controls hormones that regulate stress, such as cortisol, thyroid function, reproductive function, growth, and even milk production. One of the most common tumors that grows in this area of the brain is called a pituitary adenoma.
Pituitary tumors, and adenomas in particular, are typically benign tumors that can sometimes result in over- or under-production of normal hormones. Once you have been diagnosed with a pituitary tumor, your doctor will check your hormone function to determine if your tumor is a prolactinoma, or another type of pituitary tumor.
In most cases, there is no medical treatment for pituitary tumors, except in the case of prolactinomas, which are first treated with medicine. Small tumors (microadenomas) can typically be observed if they are not causing a hormone abnormality.
For larger tumors, called pituitary macradenomas, surgery to remove the tumor is recommended when they grow, cause pressure on the eye nerves, or cause excess hormone production not amenable to medicine.
The majority of pituitary tumors can be removed using a minimally invasive surgery called endoscopic endonasal transsphenoidal surgery. In this type of surgery, a small light and camera is used to guide removal of the tumor from the back of the nose, using special instruments to expose and remove the tumor. Transsphenoidal surgery leaves no visible scar, minimizes the risk of complications, and enables faster recovery.
How is pituitary surgery performed?
In the operating room, surgery is performed first by gently moving your normal nasal structures in order to identify the opening to the sphenoid sinus (a hollow space between your nasal cavity and the skull) to expose the sella, where the pituitary tumors arise.
The bony walls of the sphenoid sinus are enlarged to maximize exposure to the sella. The bone of the sella and at the base of the skull is carefully drilled, until the covering of the brain, or dura, is exposed. The dura is then opened, and the tumor is removed in small pieces, while taking care to preserve the normal pituitary gland.
The defect is then closed using reconstructive products, and in some cases, your own nose tissue including tissue harvested from your nasal septum. There are typically no cuts or incisions outside of the nose that are required.
This surgery is ideally done with a neurosurgeon, who does the tumor removal, and an ENT surgeon, who creates a corridor in the nose to allow for the tumor to be removed. In most cases, small tumors can be removed completely, while the ability to remove larger tumors completely depends on what structures it involves and its texture.
During recovery, you may have difficulty breathing through your nose, and will be encouraged to breath through your mouth. You will be instructed not to blow your nose, use straws, or have any pressurized air placed over your nose. You will be encouraged to drink when thirsty, and you can expect to get out of bed the day after surgery in most cases. A typical post-operative stay in the hospital is 2-3 days if there are no complications.
Risks and Recovery from Surgery
The most common risks associated with this type of surgery include hormone level changes and cerebrospinal fluid leak. After surgery, your team will monitor you closely for changes in your hormone levels, which can occur due to manipulation or damage to the pituitary gland during surgery. One of the most common hormone problems seen is called diabetes insipidus, a condition in which the salt regulating hormone vasopressin is affected, causing high urine production and salt levels.
This is most likely to occur in the first 2-3 days after surgery, while you are still in the hospital, and these levels will be watched closely. While up to 30% of patients can develop problems with the salt regulating hormone vasopressin, a majority of these cases resolve on their own or are temporary. If needed, you will be started on hormone replacement therapy, and you will be tested by your endocrinologist as an outpatient to determine how long the therapy needs to continue.
Cerebrospinal fluid leaking can commonly be seen during tumor resection. In a majority of cases, collagen based products and tissue from your nose, including in some cases a vascularized nasoseptal flap, can be used to close the opening and prevent fluid leaking after surgery.
You will be monitored after surgery for water-like dripping from the nose, resembling a faucet, which may be a sign of a cerebrospinal fluid leak. Other signs include a salty or metallic taste in the mouth, and headaches that are worse in some positions. You will be instructed to watch for these symptoms until your follow-up.
We are more than surgeons,
we are your support system.
More serious, but rarer, risks include risk of infection (resulting in meningitis), significant bleeding, such as with injury to the nearby blood vessels, or injury to the eye nerves. In most cases, the surgery can be done without significant manipulation of the brain itself, making it an ideal way to preserve brain function.
Surgery is also extremely effective at preserving and in many cases improving vision for patients who have compression of their visual structures prior to surgery. While most pituitary tumors can be removed through an endoscopic, endonasal transsphenoidal technique, some more complex tumors may require additional surgery through an opening in the top of the skull, called a craniotomy.
After you go home, you will likely have your hormone levels checked again before follow-up. You will be scheduled for follow-up with your neurosurgeon, ENT surgeon, endocrinologist, and ophthalmologist.
You will experience a sinus-type headache for the first 1-2 weeks after surgery, and will be encouraged to use a nasal saline spray to help with the dryness. By 2 weeks after surgery, you should feel significantly better, with improved nasal congestion and sinus discomfort. We recommend light activities during the 4-6 week recovery period, after which you can typically resume your normal activities.
You will continue to have MRI scans of your brain every 3-6 months after surgery initially, then typically every year for some period of time. Your doctor will discuss the need for any further surveillance or therapy with you on a case-by-case basis.
Endoscopic pituitary tumor surgery is a safe, effective, minimally invasive procedure in well-trained hands. Make sure your surgeon has advanced training in pituitary tumor surgery, and is working as part of a multi-disciplinary team.

About Dr. Rupa Juthani
Dr. Juthani has expertise in a wide range of oncologic conditions including pituitary adenomas, skull base tumors, brain metastases, and gliomas. Dr. Juthani has unique training in minimally invasive approaches including endoscopic pituitary and skull base surgery, laser surgery, Gamma Knife radiosurgery, and fluorescence guided surgery.
Recent Posts: