Failed Back surgery syndrome, failed back syndrome (FBSS) is a diagnosis given to people with a history of spinal surgery and who continue to have pain or symptoms after the surgery. FBSS is a misnomer, this is not a defined syndrome since the issues leading to the diagnosis of FBSS can be different things.
Sometimes patients feel that they initially improved after surgery but got worse again, that the pain never improved, or could be worse than before surgery. FBSS can occur after any type of spine surgery, such as spinal fusion, including cervical, thoracic, or lumbar fusion and/or decompression surgeries, which includes laminectomies and discectomies.
FBSS can be diagnosed in patients who had back surgery but continue to have symptoms that affect their quality of life, including chronic pain, or leg pain, it does not necessarily mean that the patient has ‘failed’ or the surgery has ‘failed’.
When a patient presents after previous spinal surgery with continued or worsened symptoms, re-evaluation will often include repeat Xrays, a Magnetic Resonance Image (MRI) from after surgery and if a fusion was performed, a repeat Computed Tomography (CT or CAT scan).
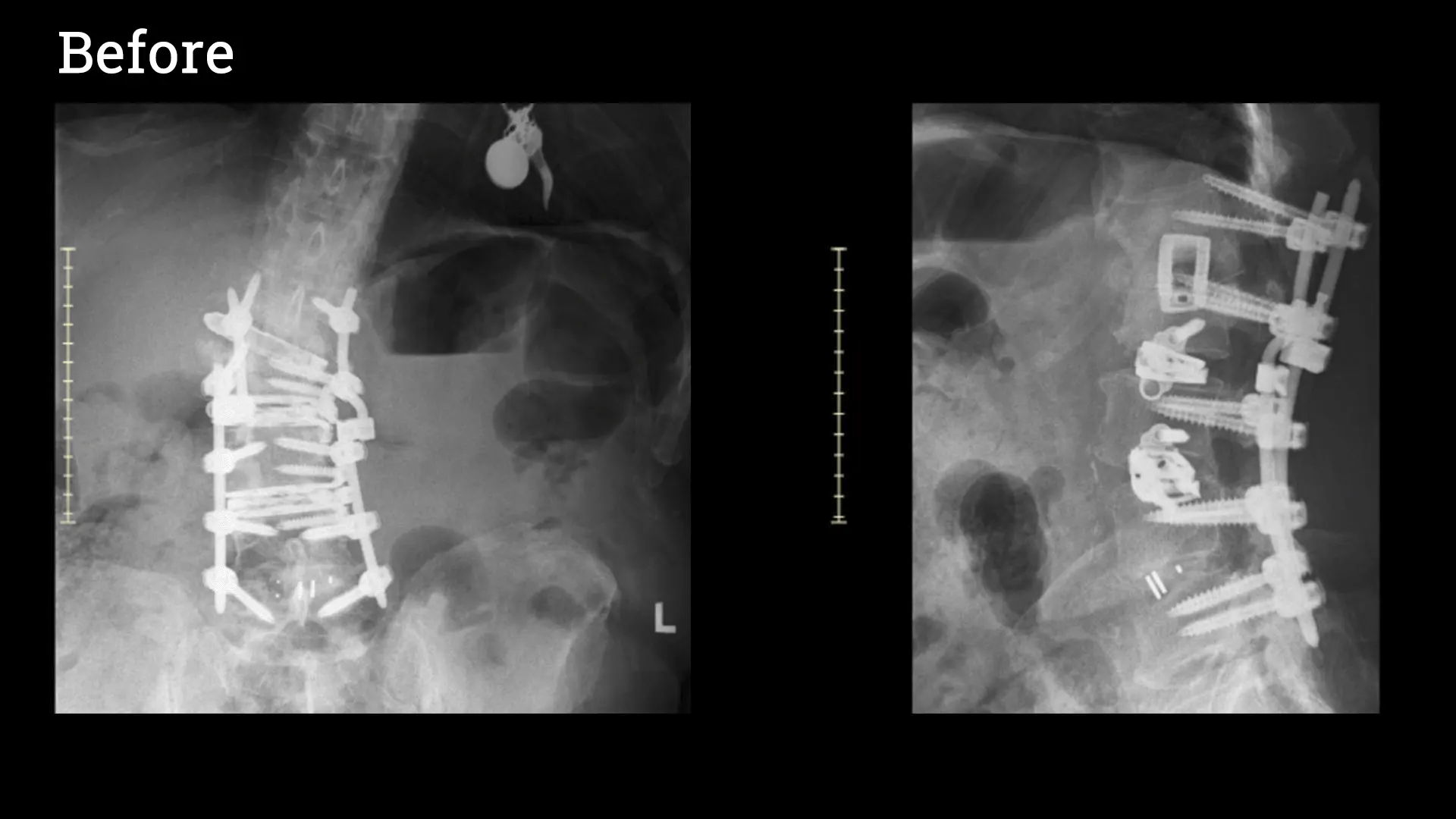
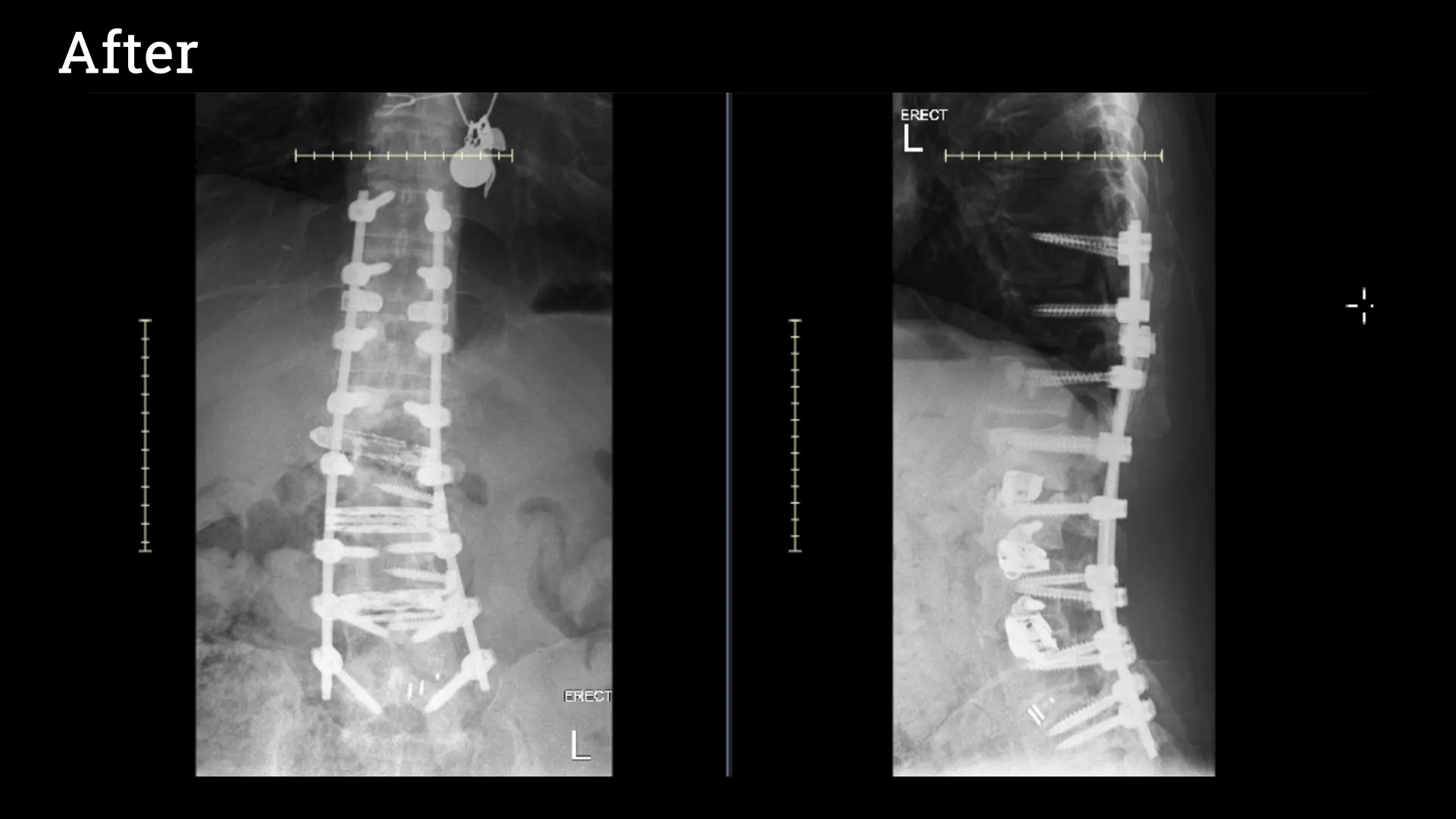
The MRI is best for evaluating the nerves, spinal cord, and soft tissues, while the CT scan is best for looking at the bones and hardware that may have been placed.
The cure or treatment for FBSS does not always mean more surgery or revision surgery is recommended, however, a repeat surgical evaluation is important to rule out potential physical or mechanical causes for the surgery to fail.
Reasons for surgery to have failed, and be able to be fixed with further surgery, usually fall into one of four categories:
- Failure of the initial surgery to fully address the pathology such as continued stenosis or compression at levels where the spinal cord or nerves were decompressed, this can include scar tissue, nerve root compression, herniated discs;
- Failure of hardware or for the bones to heal, such as hardware fracture or loosening, non-union or pseudo-arthrosis of the fusion where the bone did not grow as expected;
- Adjacent segment degeneration (ASD) or further degeneration at another level of the spine that could have been exacerbated from the surgery or developed shortly thereafter;
- Postoperative development of spinal deformity – examples include loss of curve (lordosis) from implant issues, development of a slip of the spine (this is called spondylolisthesis) that was not present prior to surgery (especially in cases of a laminectomy without fusion at multiple levels – this is called ‘post-laminectomy syndrome’), and postoperative infection can also lead to postoperative deformity.
It's time to get back
to doing what you love.
After evaluation by a spinal surgeon and the repeat imaging (MRI, CT, X rays), it will be discussed if further surgery or a revision surgery can fix the problem.
These studies can evaluate the spinal nerves, for herniated discs, for ongoing or new stenosis, for the presence of scar tissue and allows for evaluation of the spinal nerves and hardware.
In some cases, there are non-surgical interventions that can help with the ongoing pain or neurologic issues. These situations can result from nerve injury or spinal cord compression that will not always improve if it is severe enough prior surgery, from nerve injury during surgery that will take time to recover but may not always recover. These types of problems cannot always be distinguished on imaging studies.
These patients best served by further pain management or physical medicine and rehabilitation evaluation for non-surgical interventions or measures. This can include spinal cord stimulation, peripheral nerve stimulation, further injections or nerve ablations or a host of other interventions that are tailored to the specific patient.
The treatment of FBSS is multi-factorial as it depends on which of the above issues are leading to the ongoing symptoms.
The treatment of FBSS is multi-factorial as it depends on which of the above issues are leading to the ongoing symptoms.
In significant deformity cases, revision can also sometimes need multi-level fusion with bone cuts (osteotomies) to restore posture and curve to the spine.
There are also now several minimally invasive surgery options for revision surgery that may be possible after evaluation and allow for a quicker recovery with less tissue disruption and risk of further degeneration at additional levels.

About Dr. Christopher Gillis
Dr. Christopher Gillis is an accomplished neurosurgeon in Central Jersey and a proud member of Neurosurgeons of New Jersey, practicing out of their West Long Branch office conveniently located on Highway 36 West. Dr. Gillis is a fellowship trained spine surgeon out of Rush University in Chicago and his specialty is minimally invasive and complex brain and spine surgery. His clinical and research interests include developing and advancing innovative techniques for minimally invasive spine surgery, spine deformity correction, revision spine surgery, as well as robotics. Dr. Gillis’ passion is driven by helping patients regain their quality of life after suffering from disabling medical conditions. He is currently accepting new patients.
Recent Posts: